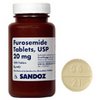
Pharmacodynamics
The drug Furosemide is a strong and fast-acting diuretic, which is a derivative of sulfonamide.
The drug Furosemide blocks the system of transport of sodium ions (Na +) potassium (K +) chlorine (Сl-) in the thick segment of the ascending loop of Henle loop, and therefore its diuretic effect depends on the drug entering the lumen of the renal tubules (due to the mechanism of anion transport) . The diuretic effect of the drug Furosemide is associated with inhibition of sodium chloride reabsorption in this section of the loop of Henle. Secondary effects with respect to an increase in sodium excretion are: an increase in the amount of urine secreted (due to osmotically bound water) and an increase in potassium secretion in the distal part of the renal tubule. At the same time increases the excretion of calcium and magnesium ions. When the canalicular secretion of furosemide decreases or when furosemide binds to albumin present in the tubule lumen (for example, in nephrotic syndrome), the effect of furosemide decreases.
During the course taking of the drug Furosemide, its diuretic activity does not decrease, since furosemide interrupts the canalotis-glomerular feedback in Macula densa (the tubular structure closely associated with the juxtaglomerular complex). The drug Furosemide induces a dose-dependent stimulation of the renin-angiotensin-aldosterone system. In heart failure, the drug Furosemide quickly reduces preload (due to the expansion of the veins), decreases the pressure in the pulmonary artery and the filling pressure of the left ventricle. This rapidly developing effect appears to be mediated through the effects of prostaglandins and therefore the condition for its development is the absence of impairments in the synthesis of prostaglandins, in addition to which this effect also requires sufficient preservation of renal function. The drug Furosemide has an antihypertensive effect, which is caused by an increase in sodium excretion, a decrease in circulating blood volume and a decrease in the reaction of vascular smooth muscle to vasoconstrictive stimuli (due to the natriuretic effect, furosemide reduces the response of vascular to catecholamine, whose concentration in patients with arterial hypertension is increased). After ingestion of 40 mg of the drug Furosemide diuretic effect develops within 60 minutes and lasts about 3-6 hours.
In healthy volunteers who received from 10 to 100 mg of the drug Furosemide, a dose-dependent increase in diuresis and natriuresis was observed.
Pharmacokinetics
Furosemide is rapidly absorbed in the gastrointestinal tract. Its tmax. (time to reach maximum concentration in the blood) is from 1 to 1.5 hours. The bioavailability of furosemide in healthy volunteers is approximately 50-70%. In patients, the bioavailability of the drug Furosemide can be reduced by up to 30%, since it can be affected by various factors, including the underlying disease. The volume of distribution of furosemide is 0.1-0.2 l / kg body weight. Furosemide binds to plasma proteins (more than 98%), mainly albumin. Furosemide is excreted mainly in unchanged form and, mainly, by secretion in the proximal tubule. The gluconated metabolites of furosemide account for 10–20% of the renal excreted drug. The remaining dose is excreted through the intestines, apparently by biliary secretion. The final half-life of furosemide is approximately 1-1.5 hours. Furosemide penetrates the placental barrier and is secreted into the mother's milk. Its concentrations in the fetus and newborn are the same as in the mother.
Features of pharmacokinetics in certain groups of patients
In renal failure, the elimination of furosemide is slowed down, and the half-life is increased; with severe renal failure, the final half-life may increase to 24 hours. In nephrotic syndrome, a decrease in plasma concentrations of proteins leads to an increase in the concentrations of unbound furosemide (its free fraction), and therefore the risk of ototoxic action increases. On the other hand, the diuretic effect of furosemide in these patients may be reduced due to the binding of furosemide to albumin in the tubules and a decrease in the tubular secretion of furosemide.
In hemodialysis and peritoneal dialysis and continuous ambulatory peritoneal dialysis, furosemide is not significantly excreted.
In liver failure, the half-life of furosemide is increased by 30-90% mainly due to an increase in the volume of distribution. Pharmacokinetic indicators in this category of patients can vary greatly.
In heart failure, severe hypertension, and in elderly patients, the elimination of furosemide slows down due to a decrease in renal function.
Indications
- edematous syndrome in chronic heart failure;
- edematous syndrome in chronic renal failure;
- acute renal failure, including those during pregnancy and burns (to maintain fluid excretion);
- edema syndrome in nephrotic syndrome (in nephrotic syndrome in the foreground is the treatment of the underlying disease);
- edematous syndrome in liver diseases (if necessary, in addition to treatment with aldosterone antagonists);
- arterial hypertension.
Contraindications
- Hypersensitivity to the active substance and to any of the excipients of the drug; in patients with allergy to sulfonamides (sulfanilamide antimicrobial agents or sulfonylurea derivatives), since it is possible to develop a "cross-over" allergy to furosemide;
- Renal failure with anuria (in the absence of a response to the reception of furosemide);
- Hepatic coma and precoma associated with hepatic encephalopathy;
- Severe hypokalemia;
- Severe hyponatremia;
- Hypovolemia (with a decrease in blood pressure or without a decrease in blood pressure) or degicration;
- Pronounced violations of urine outflow of any etiology, including unilateral damage to the urinary tract;
- Intoxication with cardiac glycosides;
- Acute glomerulonephritis;
- Decompensated aortic and mitral stenosis, hypertrophic obstructive cardiomyopathy;
- Increase in central venous pressure (over 10 mmHg);
- Children's age up to 3 years (solid dosage form);
- Pregnancy;
- Breastfeeding period.
Carefully
- With arterial hypotension;
- In conditions where an excessive reduction in blood pressure is particularly dangerous (severe stenosis of the coronary and / or cerebral arteries);
- In acute myocardial infarction (increased risk of cardiogenic shock);
- With latent or manifest diabetes mellitus;
- With gout;
- With hepatorenal syndrome (that is, with functional renal failure associated with liver disease);
- With hypoproteinemia (for example, with nephrotic syndrome, when it is possible to reduce the diuretic effect and increase the risk of the development of the ototoxic effect of furosemide); dose selection in such patients should be carried out with extreme caution;
- With partial obstruction of the urinary tract (prostatic hyperplasia, narrowing of the urethra);
- With an increased risk of developing disorders of water-electrolyte balance and acid-base state or in case of significant fluid loss (vomiting, diarrhea, excessive sweating - monitoring of the state of water-electrolyte balance and acid-base state and, if necessary, correction of their disorders before use of furosemide);
- With pancreatitis;
- With ventricular arrhythmias in history;
- With systemic lupus erythematosus;
- With the simultaneous use of risperidone in elderly patients with dementia (risk of increased mortality).
Symptomatic arterial hypotension, leading to dizziness, fainting, or loss of consciousness, can occur in patients receiving furosemide, especially: in elderly patients; in patients taking other drugs that may lead to arterial hypotension; as well as in patients with other diseases that carry the risk of arterial hypotension. When treating such patients, care should be taken and / or they may need to lower the dose of furosemide.
Use during pregnancy and during breastfeeding
Furosemide penetrates the placental barrier, so it should not be used during pregnancy without strict medical indications.
If, for health reasons, the drug Furosemide is used in pregnant women, careful monitoring of the condition and development of the fetus is necessary.
During breastfeeding, taking the drug Furosemide is contraindicated, as it can suppress lactation. Women, if they take the drug Furosemide, should stop breastfeeding.
Dosage and administration
General recommendations
Tablets should be taken on an empty stomach, without chewing and drinking plenty of water.
When using the drug Furosemide is recommended to use it in the smallest doses, sufficient to achieve the desired therapeutic effect.
The recommended maximum daily dose for adults is 1500 mg, and in children - 40 mg.
The duration of treatment is determined by the doctor individually, depending on the evidence.
Special recommendations for dosing regimen
Children
In children, the recommended daily intake for oral administration is 2 mg / kg body weight (but not more than 40 mg per day).
Adults
Edematous syndrome in liver diseases
The drug Furosemide is used in addition to treatment with aldosterone antagonists in case of their lack of effectiveness. To prevent the development of complications, such as impaired orthostatic regulation of blood circulation, or impaired water-electrolyte balance, or acid-base condition, careful dose selection is required so that fluid loss occurs gradually (at the beginning of treatment, fluid loss is possible to approximately 0.5 kg body per day). The recommended initial dose is 20-80 mg per day. It can be adjusted depending on the response of the patient. The daily dose can be applied 1 time per day or divided into 2 doses.

Edematous syndrome in chronic renal failure
The natriuretic reaction to furosemide depends on several factors, such as the severity of renal failure and the sodium content in the blood, so the dose effect cannot be accurately predicted. Patients with chronic renal failure require careful dose selection, by gradually increasing it so that fluid loss occurs gradually (at the beginning of treatment, loss of fluid is possible to approximately 2 liters per day, approximately 280 mmol of Na + per day).
The recommended starting dose is 40-80 mg per day. The required dose is selected depending on the diuretic response. The entire daily dose should be taken once or divided into two doses. In patients on hemodialysis, the maintenance dose is usually 250–1500 mg / day.
Acute renal failure (to maintain fluid clearance)
Before starting treatment with Furosemide, hypovolemia, arterial hypotension and significant disorders of water-electrolyte balance and / or acid-base status should be eliminated. Treatment begins with intravenous administration of the drug Furosemide. The recommended starting dose is 40 mg intravenously. If this does not achieve the desired diuretic effect, then the drug Furosemide can be administered as a continuous intravenous infusion, starting at a rate of 50–100 mg per hour. It is recommended as soon as possible to transfer the patient from intravenous administration of the drug Furosemide to taking the tablets of the drug Furosemide (the dose of the tablets depends on the selected intravenous dose).
Edema in nephrotic syndrome
The recommended initial dose is 40-80 mg per day. The required dose is selected depending on the diuretic response. The daily dose can be taken in a single dose or divided into several doses.
Edematous syndrome in chronic heart failure
The recommended initial dose is 20-80 mg per day. The required dose is selected depending on the diuretic response. It is recommended that the daily dose should be divided into two or three doses.
Arterial hypertension
The drug Furosemide can be used in monotherapy or in combination with other antihypertensive drugs.
The usual maintenance dose is 20–40 mg daily. With hypertension in combination with chronic renal failure, it may be necessary to use higher doses of the drug Furosemide.
Cautions, therapy control
Before starting treatment with the drug Furosemide, it is necessary to exclude the presence of pronounced violations of the outflow of urine, including unilateral ones. Patients with a partial violation of the outflow of urine need careful observation, especially at the beginning of treatment with the drug Furosemide.
During treatment with Furosemide, regular monitoring of sodium, potassium and serum creatinine levels is required; especially careful monitoring should be carried out in patients with a high risk of developing disorders of water and electrolyte balance in cases of additional fluid and electrolyte losses (for example, due to vomiting, diarrhea, or intense sweating). Before and during treatment with Furosemide, it is necessary to control and, in case of occurrence, eliminate hypovolemia or dehydration, as well as clinically significant impairments of water-electrolyte balance and / or acid-base state, which may require a short-term cessation of treatment with Furosemide.
When treating with Furosemide, it is always advisable to eat foods rich in potassium (lean meat, potatoes, bananas, tomatoes, cauliflower, spinach, dried fruits, etc.). In some cases, it may be shown the administration of potassium preparations or the prescription of potassium-sparing drugs.
In patients with hypoproteinemia, for example, associated with nephrotic syndrome, a decrease in the efficacy of furosemide and an increase in its ototoxicity is possible. A careful dose increase is required.
There was a high incidence of deaths in elderly patients who were simultaneously treated with risperidone and furosemide, compared with patients who received either only furosemide or only risperidone. Pharmacophysiological mechanism of this effect is not installed. The simultaneous use of risperidone with other diuretics (mainly low doses of thiazide diuretics) was not associated with an increase in mortality in elderly patients with dementia.
In elderly patients with dementia, care should be taken, carefully weighing the balance of benefits and risks, to prescribe furosemide and risperidone at the same time. Since dehydration is a common risk factor for increased mortality, when deciding on the use of this combination in elderly patients with dementia, dehydration of the patient should be avoided. There is a possibility of weighting or exacerbation of systemic lupus erythematosus. Selection of the dosing regimen for patients with ascites on the background of cirrhosis should be carried out in the hospital (violations of water and electrolyte balance may lead to the development of hepatic coma).
Furosemide contains lactose monohydrate ‚therefore patients with lactose intolerance, lactase deficiency, glucose-galactose malabsorption syndrome should not take this drug.
The preparation contains wheat starch in an amount that is safe for use in patients with celiac disease (gluten enteropathy). Patients with a history of allergy to wheat starch (other than celiac disease) should not use this drug.
Influence on ability to steer vehicles, mechanisms
Some side effects (for example, a significant reduction in blood pressure) can impair the ability to concentrate and reduce psychomotor reactions, which can be dangerous when driving a car or doing other potentially dangerous activities. This applies particularly to the period of initiation of treatment or increasing the dose of the drug, as well as to the cases of simultaneous administration of antihypertensive drugs or alcohol. In such cases, it is not recommended to drive vehicles or engage in potentially hazardous activities.
Overdose
If an overdose is suspected, it is imperative that you seek medical attention, as in the event of an overdose, certain therapeutic measures may be required.
The clinical picture of an acute or chronic overdose of a drug depends mainly on the degree and consequences of fluid and electrolyte loss. Overdose may be manifested by hypovolemia, dehydration, hemoconcentration, abnormal heart rhythm and conduction (including atrioventricular block and ventricular fibrillation). Symptoms of these disorders are marked reduction in blood pressure, progressive to the development of shock, acute renal failure, thrombosis, delirious state, flaccid paralysis, apathy and confusion.
There is no specific antidote. If a little time has passed after ingestion, to reduce the absorption of furosemide from the gastrointestinal tract, you should try to induce vomiting or gastric lavage, and then ingest activated charcoal.
The treatment is aimed at correcting clinically significant impairments of water-electrolyte balance and acid-base status under the control of electrolyte content in blood serum, indicators of acid-base status, hematocrit, as well as the prevention or therapy of possible serious complications developing on the background of these disorders.
 US
US AU
AU UK
UK DE
DE FR
FR IT
IT ES
ES